How to sleep with a broken shoulder in a sling (or without)?
What is the best sleeping position for broken humerus?
I draw upon my experience as a physical therapist to assist you in finding the best positions while awaiting healing!
Feel free to share your experiences, insights, or questions in the comments section below!
Take-home message: The best sleeping position is the one that suits you the most, and you won’t risk worsening your problem by sleeping on the painful shoulder (so if it’s your preferred position, you can keep it).
Happy reading 🙂!
Last update: October 2023
Disclaimer: Affiliate links. Complete disclosure in legal notices.
Written by Nelly Darbois, a trained physical therapist & scientific writer
If you would like more information about this rehabilitation period, I have dedicated an eBook to this topic 🙂!
Summary
Why is it difficult to sleep after a humerus fracture?
Sleeping with a humerus fracture can disrupt sleep in various ways:
- Pain can hinder falling asleep at the beginning of the night or later after waking up.
- Pain can lead to multiple awakenings during the night.
- It can also prevent entering a sufficiently restorative sleep.
The issue is that the less one sleeps, the more sensitive they become to pain [Chang, 2022], and the more challenging it is to sleep. It’s a vicious cycle.
So, you are right to wonder: how can I ensure that my shoulder fracture disturbs my sleep as little as possible (or not at all)?
To address this question, I suggest examining the following two questions in light of international scientific literature:
- Is there a specific solution for sleeping better with a shoulder fracture while awaiting consolidation?
- How can you sleep better with pain, no matter where it’s located?
You’re not alone! 41% of patients who have had a humerus fracture report difficulty sleeping three months after the fracture (Shulman 2015).

Sleeping Better with a Humerus Fracture: A Specific Solution?
Is there anything specific to do to make your shoulder break less bothersome at night? Unfortunately, after thoroughly reviewing international scientific literature, I haven’t found anything of the sort.
That being said, there are, of course, some fundamental steps, which you’ve likely already considered, worth briefly discussing. These include:
- Changing sleeping positions.
- Changing bedding (especially mattresses and pillows).
Changing Sleeping Positions?
Let’s clarify from the outset that whether you want it or not, there’s a good chance you’ll automatically change positions during the night. This is the case for the majority of people who, on average, switch positions every hour (Skarpsno, 2017).
In other words, the question is whether there’s a preferred position for falling asleep, either at the beginning or during the night if you wake up.
The answer is: the best position for falling asleep (or falling back asleep) is the one that suits you best.
This holds true even though you’ll come across numerous web articles suggesting that sleeping on your back, on your stomach, etc., is better. However, there is no credible scientific study supporting these recommendations.
Source : Skarpsno 2017
In my experience as a physical therapist, I’ve noticed some common preferences that patients tend to lean towards.
Many patients prefer to sleep with their arm in the brace or sling provided by their healthcare provider. This is because the brace helps limit movement and stabilize the injured area, which can help reduce pain and discomfort during sleep.
While it might not be the most comfortable thing to wear, it does serve a purpose in maintaining proper alignment and minimizing unnecessary strain on the injured arm.
Here are some explanations to put the sling correctly:
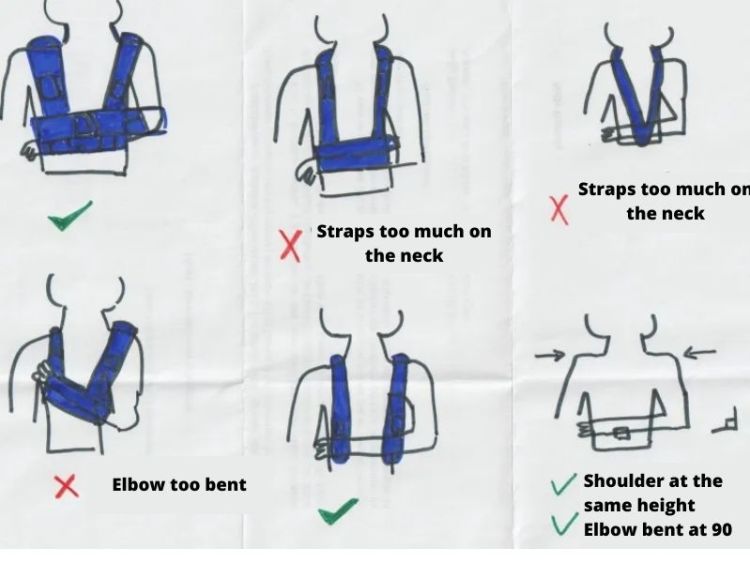
Additionally, patients often find that sleeping on their back or in a slightly elevated position with the upper body propped up by pillows can alleviate some of the discomfort.
Can you sleep on side with broken humerus?
Even for lying on the side where you have discomfort, there’s no evidence that it could worsen the issue. (Note that this holds true for any sleeping position.)
So, if that’s your preferred position for falling asleep, you don’t necessarily need to change it.
The pressure on the shoulder won’t worsen the fracture. It’s only strong impact or repetitive large movements that can do that. So, you can sleep on it even before the consolidation.
However, it often hurts to sleep on the fractured humerus, especially during the first few weeks.
Changing Mattresses or Pillows?
Here as well, there is no scientific evidence to suggest that changing your mattress or pillow can help improve sleep in the case of a fracture.
However, it’s possible that in your specific case, a particular mattress or pillow may be more suitable for you than others. It’s possible, and you’re free to experiment (although properly trying out a new mattress can be a bit complicated; indeed, it’s challenging to go back…).
Note: nursing pillows can be a cost-effective option for trying out new sleeping configurations. They are highly adaptable.
In summary:
- The best sleeping position with a humerus fracture is the one that suits you best.
- You won’t risk exacerbating your problem by sleeping on the painful shoulder (if that’s your preferred position).
- There is no scientific basis to recommend a specific mattress or pillow.
See also: My Opinion (+ What studies say) on Memory Foam Mattress
Reducing stress?
When researchers monitor the sleep of people who have fractured their humerus, they observe that sleep quality isn’t necessarily worse among those who have slower recoveries.
Sleep tends to be less restful in individuals who are stressed, anxious, or depressed.
Therefore, implementing solutions to reduce your stress is likely to significantly improve your sleep.
Source: Shulman 2015
How to get out of bed with broken shoulder?
Getting out of bed with a broken shoulder can be challenging, but here are some steps to help make it easier!
- Sleep on the Uninjured Side: If possible, try to sleep on the side opposite your broken humerus. This can make it easier to get out of bed on your own.
- Use a Bed Rail or Transfer Bar: If you have a bed rail or transfer bar installed on your bed, use it to assist with getting in and out of bed safely. These devices provide stable support for getting up.
- Slide to the Edge: Start by sliding your body towards the edge of the bed, keeping your legs extended. Use your uninjured arm to help push your body closer to the edge.
- Roll Onto Your Side: Once you are close to the edge, carefully roll onto your uninjured side. Use your legs to help with the movement.
- Push Up: With your uninjured arm, push your body up to a seated position on the edge of the bed. Take your time and move slowly to avoid any sudden jolts or jerks that could strain your injured shoulder.
- Seek Assistance If Needed: If you find it too challenging to get out of bed on your own, don’t hesitate to ask for help from a caregiver or family member. Your physical therapist can also show you how to do it, especially if you have a home-based therapist who can demonstrate in your actual environment!
How to Sleep Better with Pain, with or without broken humerus?
The overall strategy to consider for nighttime pain that includes three steps (Perrig, 2011):
- First, ensure that the basic principles of good sleep hygiene are followed.
- Next, consider non-pharmacological approaches.
- Then, if necessary, explore pharmacological approaches.
I’m going to detail all of this!
Recommandations for sleep hygiene
Here is the list of the main recommendations for sleep hygiene that have been reviewed in studies:
- Avoid naps longer than one or two hours during the day.
- Go to bed at the same time every day.
- Wake up at the same time every day.
- Avoid vigorous physical exercise that makes you sweat within an hour before bedtime.
- Avoid staying in bed longer than necessary in the morning (no more than two or three times a week).
- Avoid stimulating activities just before bedtime.
- Avoid going to bed feeling stressed, angry, upset, or nervous (personal note #1: easier said than done!).
- Have a comfortable mattress.
- Create a comfortable bedroom environment (moderate temperature, as dark as possible, minimal noise).
- Avoid thinking, planning, or worrying once in bed (personal note #2: again, easier said than done!).
- Avoid nicotine, caffeine, and alcohol.
- Engage in regular physical activity.
So, do these recommendations work? The simple answer is that we don’t know for sure.
On one hand, there are good reasons to believe that they may work. On the other hand, very few high-quality studies have investigated whether they actually work in real life (and the results are inconclusive).
In practice, I think it may be worth trying (or re-trying) some of these recommendations.
In summary:
- Sleep hygiene recommendations found online are not well-studied by science.
- However, there are good reasons to believe that these recommendations are still worth our attention.
- In practice, trying (or re-trying) some of these recommendations seems reasonable.
Source: Irish, 2015, Gupta, 2023
Improving sleep without medication
There are numerous non-pharmacological approaches available to treat pain-related insomnia. You might have even tried several of them. Among these approaches, several have been the subject of scientific studies.
In 2022, researchers reviewed all these studies (Whale, 2022).
Without going into detail, what are the conclusions of this study? Its conclusions are as follows:
- Behavioral and cognitive therapies are the most well-documented and promising approach.
- However, there is a lack of evidence regarding their long-term effectiveness.
- All other approaches have been insufficiently studied to make any confident declarations.
Now, let’s take a look at the approaches involving medications.
Improving sleep with medication
Studies on medication-based approaches for pain-related insomnia were comprehensively reviewed in 2021 (Herrero Babiloni, 2021). Researchers examined all scientific works that studied:
- The effect of pain medications on insomnia.
- The effect of insomnia medications on pain.
As mentioned in a previous section, unfortunately, there is no specific study on the pain of a broken humerus. To date, the best we can do is to look at what is said for insomnia related to chronic back pain, as this is where most studies are found.
Here is my summary of the latest literature review on this topic (Craige, 2022):
- Medication-based approaches improve sleep in individuals with chronic back pain.
- However, the effects are very small, so small that one might wonder if they are genuinely significant.
- Consequently, professionals should steer their patients towards non-pharmacological approaches instead.
- However, it’s worth noting that the studies we reviewed to conclude all of this are limited in number and of relatively poor quality.
Conclusion on Optimal Sleeping Positions for a Broken Humerus
🛌 There is no specific scientific evidence regarding the best sleeping positions with a broken humerus.Your sleeping positions should be chosen based on your personal comfort and preference.
There is no indication that sleeping on your affected shoulder would worsen the fracture!
😴 Basic sleep hygiene practices should be considered, such as avoiding intense physical activity right before bedtime, maintaining a consistent sleep schedule, and creating a comfortable sleeping environment.
💊 Medication-based approaches for pain-related insomnia have been studied, primarily in the context of chronic back pain. While they may offer slight improvements in sleep, the effects are generally small.
***
Here’s what I wanted to tell you about this! I wish you a very good recovery! Do you have any comments or questions? Your comments are welcome 🙂 !
If you feel the need to learn more about the recovery period after this type of fracture, I wrote this guide in eBook format:
You may also like:
- How long does last healing and recovery after broken humerus?
- Fracture of the humeral head : recovery time
📚 SOURCES
Chang JR, Fu SN, Li X, Li SX, Wang X, Zhou Z, Pinto SM, Samartzis D, Karppinen J, Wong AY. The differential effects of sleep deprivation on pain perception in individuals with or without chronic pain: A systematic review and meta-analysis. Sleep Med Rev. 2022 Dec;66:101695. doi: 10.1016/j.smrv.2022.101695. Epub 2022 Sep 27. PMID: 36334461.
Shulman BS, Liporace FA, Davidovitch RI, Karia R, Egol KA. Sleep disturbance after fracture is related to emotional well-being rather than functional result. J Orthop Trauma. 2015 Mar;29(3):e146-50. doi: 10.1097/BOT.0000000000000217. PMID: 25072285.
Does your sleeping position affect your shoulder pain?. J Health Sci Med / JHSM. 2022; 5(3): 782-788.
Skarpsno ES, Mork PJ, Nilsen TIL, Holtermann A. Sleep positions and nocturnal body movements based on free-living accelerometer recordings: association with demographics, lifestyle, and insomnia symptoms. Nat Sci Sleep. 2017 Nov 1;9:267-275. doi: 10.2147/NSS.S145777. PMID: 29138608; PMCID: PMC5677378.
Perrig S, Espa-Cervena K, Pépin JL. [Sleep disorder and pain: the good hypnotic]. Revue Medicale Suisse. 2011 Jun;7(301):1414-8, 1420. PMID: 21815499.
Irish LA, Kline CE, Gunn HE, Buysse DJ, Hall MH. The role of sleep hygiene in promoting public health: A review of empirical evidence. Sleep Med Rev. 2015 Aug;22:23-36. doi: 10.1016/j.smrv.2014.10.001. Epub 2014 Oct 16. PMID: 25454674; PMCID: PMC4400203.
Gupta CC, Sprajcer M, Johnston-Devin C, et al Sleep hygiene strategies for individuals with chronic pain: a scoping review. BMJ Open 2023;13:e060401. doi: 10.1136/bmjopen-2021-060401
Herrero Babiloni A, Beetz G, Bruneau A, Martel MO, Cistulli PA, Nixdorf DR, Conway JM, Lavigne GJ. Multitargeting the sleep-pain interaction with pharmacological approaches: A narrative review with suggestions on new avenues of investigation. Sleep Med Rev. 2021 Oct;59:101459. doi: 10.1016/j.smrv.2021.101459. Epub 2021 Jan 28. PMID: 33601274.

Written by Nelly Darbois
I enjoy writing articles that answer your questions, drawing on my experience as a physiotherapist and scientific writer, as well as extensive research in international scientific literature.
I live in the French Alps☀️🏔️, where I enjoy the simple pleasures of life (+ I’m a Wikipedia consultant and the founder of Wikiconsult).




