What rehabilitation, duration of immobilization, and healing time are recommended after a fracture of the humeral head?
It is quite common to have these questions after experiencing such a fracture. Especially considering that, until it happens to us, we might not have known that this part of the arm could break!
In this article, I address all the most frequently asked questions from internet users and my patients about fractures of the humeral head. I rely on:
- my experience as a physical therapist;
- in-depth research in international scientific publications (all references at the end of the article).
Happy reading 🙂!
Last update: November 2023
Disclaimer: Affiliate links. Complete disclosure in legal notices.
Written by Nelly Darbois, physical therapist and scientific writer
If you would like more information about this rehabilitation period & exercices, I have dedicated an eBook to this topic 🙂!
Summary
What does a fracture of the humeral head look like?
The humerus is one of the bones in the human body that fractures most frequently, and it can break in different locations.
One of these locations is what we call the head of the humerus, proximal humeral head, or humeral head (it means exactly the same thing).
This location frequently fractures in women over 80 years old (1150 cases per 100,000 people) (Jaeger 2012).
There is a humeral head at the level of the right shoulder and a humeral head at the level of the left shoulder, and both can be broken.
Generally, an X-ray (sometimes a CT scan or an MRI) detects the precise location of the fracture. It also determines the type of humeral head fracture:
- Displaced or non-displaced? There is displacement of the fracture when the two bone fragments are widely separated. There is no displacement when the two bone fragments still touch at the fracture line. Non-displaced fractures generally recover even faster than displaced ones.
- Open or closed fracture? Sometimes the bone is significantly deviated from its axis and pierces the skin: this is called an open fracture. Closed fractures are much more common.
- Simple or complex/comminuted fracture? Sometimes the humeral head is broken rather simply, with a single fracture line. More rarely, the head is broken in multiple places, with multiple bone fragments: in this case, it is a complex or comminuted fracture, which may take a bit longer to heal and recover.
- Crack or fracture? We speak of a crack when the fracture line is very discreet. This will likely heal even faster, all else being equal.
You will learn more about the specific type of your humeral head fracture by reading:
- The X-ray report;
- The medical letter following your visit to the doctor or emergency room. This letter is often addressed to your general practitioner and sometimes to the physiotherapist.
Regardless of the specific type of humeral head fracture, the follow-up generally follows the same broad principles, which I will detail for you here.
What is the treatment for a humeral head fracture?
Following a fall, an accident, or an impact on the arm, you experienced intense pain.
Generally, you sought medical attention at the emergency room. Less frequently, you may visit your doctor, sometimes a few days later.
Faced with your symptoms (pain, sometimes deformation of the bone, bruising, or swelling), doctors decide to perform an X-ray. This is where the diagnosis of a humeral head fracture is established.
The X-ray is often reviewed by an orthopedic surgeon, specialists in broken bones and injured joints. Although sometimes, the interpretation of the X-ray by the emergency physician or general practitioner is sufficient.
They will decide on the treatment based on your overall health, lifestyle, the type of fracture, other issues you may have, and their own approach to treatment. There are three main treatment approaches, which may be combined or used individually:
- Conservative treatment alone: usually involves immobilization with a sling-type brace.
- Surgical treatment: an operation.
- Rehabilitation: often performed by physical therapists, sometimes by occupational therapists. Most commonly in private practices or home-based physical therapy, sometimes in a rehabilitation center (depending on your overall health and lifestyle).
Conservative / Orthopedic Treatment = Duration of Immobilization
Fractures in this part of the humerus often do not require surgery most of the time: 78% of these fractures are treated with a simple brace (Launonen 2015).
In this case, you will likely be prescribed a sling or a brace attached to the body. Reimbursable if you have a prescription from a physiotherapist or doctor.
There are more or less encompassing braces.
The more encompassing the brace, covering much of the arm, forearm, and shoulder, the less you move. This is not necessarily what is sought.
It’s essential to find the right balance:
- Not too much movement to alleviate pain and encourage consolidation.
- Not too much immobilization to avoid stiffness, loss of strength, and functional capabilities.
For simple fractures, non-displaced, without any particular complications (the most common), I typically recommend a simple sling to my patients.
Your (para)medical team will provide you with information on:
- How to put it on correctly.
- How long to keep it on.
- At what times of the day you can take it off.
Here are some explanations (and an attempt at illustration 🤭) on how to put it on correctly:
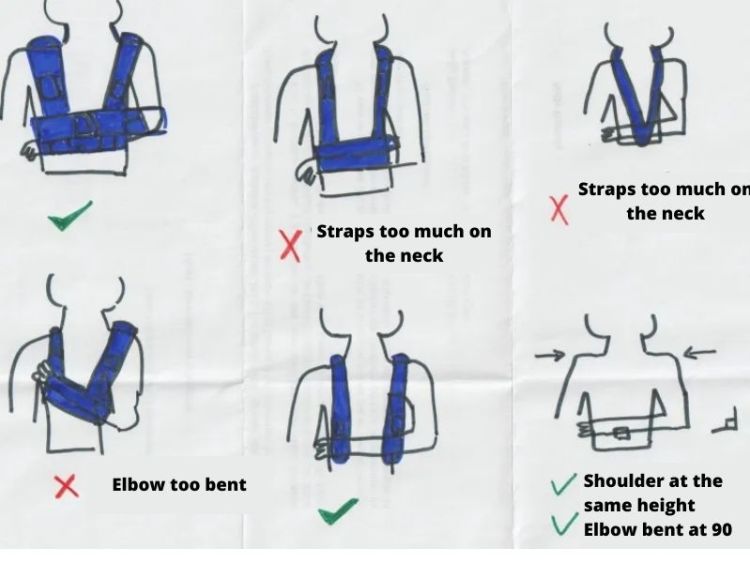
What is the recommended duration of immobilization?
Generally, you may have been told 2 weeks, 4 weeks, 6 weeks, or until the follow-up X-ray.
You can also discuss this directly with your physiotherapist and gradually start tapering off the brace when appropriate.
Should the brace be worn at night?
Most people prefer to wear it at night as it limits arm movements and reduces the risk of being awakened by pain.
Most often, your primary treatment will involve limiting shoulder and/or elbow movements to facilitate healing. This is often achieved through rest and wearing a brace for a few weeks.
Surgical Treatment = Operation
In some cases, surgery is necessary, especially if you have a displaced or comminuted fracture (although it’s not automatic: Jaeger 2012).
Surgeons will typically perform:
- Osteosynthesis with a plate and screws.
- An anatomical or reverse shoulder prosthesis (typically in individuals over 75 years old, as it restricts shoulder movements more: Jaeger 2012).

We don’t know if one type of surgical intervention is more effective than another (Cochrane 2022).
Does operating on a displaced fracture increase the chances of better recovery and a higher quality of life afterward? It’s challenging to have high-quality comparative data on this topic. Existing data show no differences in these parameters (Cochrane 2022).
The operation is performed under general anesthesia, either on the same day as the fracture or in the days following.
The shoulder replacement is typically kept “for life” unless any issues arise. The same applies to plates and screws if they don’t cause any problems.
You will likely still wear a brace attached to the body (orthopedic treatment) even if you undergo surgery.
Depending on the type of fracture, your lifestyle, your health, and the practices of the professionals you consult, you may also undergo surgery for your radial head fracture. The goal of the operation is to stabilize the fracture, often accompanied by immobilization with a brace.
Rehabilitation of a Humerus Head Fracture
After a humerus head fracture, most people in France are prescribed physiotherapy sessions. The prescription is issued:
- either immediately after leaving the emergency room or trauma service;
- or during your follow-up appointment approximately 6 weeks after the fracture.
Here’s what I recommend:
- consult a physiotherapist for an assessment in the days following the fracture;
- depending on your overall health, the fracture, and your apprehension, the physiotherapist may suggest seeing you only in 1 or 2 weeks (or even 6 weeks), rarely twice a week.
During the healing phase
During the phase when you have a brace, physiotherapists will:
- answer your questions (often numerous, which is normal!);
- reassure you about the issues you’re facing and propose solutions, such as pain relief or better sleep;
- show you what you can and cannot do during this phase to encourage consolidation without becoming too stiff.
Some people will mobilize your shoulder (lifting the arm, moving it backward, to the side) from the first days following the fracture. And they will show you how to do it gently and gradually on your own, sometimes several times a day. This is called early mobilization.
Other physiotherapists may recommend not moving at all during the 6 weeks of “immobilization.” At most, they will have you remove the brace with them to straighten the elbow for a moment.
In my practice, I discuss these two options with my patients. I recommend opting for early mobilization as soon as they are less painful. We gradually implement this in the days or weeks following the operation. I adapt to their pace, pain levels, and apprehension (well, I try!)
I prefer self-rehabilitation: there are 24 hours in each day. Your physiotherapist spends a maximum of 30 minutes with you 2/3 times a week. What matters most is what you do in the remaining 23 hours and 30 minutes!
❌ Self-rehabilitation does not mean doing exercises non-stop all day!
✅ It simply means staying active, knowing what you can do or should avoid, and gradually reintroducing functional movements into your daily life, adapting based on the signals your body sends.
The data available on the progress of people mobilized early (within the first 3 weeks) compared to those who are not mobilized are of low quality and do not allow us to say if one approach is better than another. (Cochrane 2022)
In any case, you can:
- bend and move your fingers, hands, and wrist;
- bend and straighten the elbow.
If you would like more information about this rehabilitation period & exercices, I have dedicated an eBook to this topic 🙂!
After Bone Healing
Once consolidation is achieved, you can gradually become more active with your arm. The goal is to regain the range of motion and strength you had before, over a few weeks or months.
And most importantly, to be able to use your arm again in all the activities you did before!
During healing, the aim is to prevent you from losing too much flexibility and strength in your arms (and other parts of the body). Once consolidation is achieved, the goal is to gradually regain the ability to use your arm as before.
Pain: Is it normal after a humerus head fracture?
It is common to experience pain in the days following the fracture, and even in the weeks that follow.
Pain can fluctuate: decrease, then increase, without any particular reason. It can be present at rest (doing nothing), during movement, at night, or during the day.
Pain does not mean there is a complication or that you are not still consolidating.
Several measures can be taken to relieve or limit pain:
- find more comfortable positions, especially with the help of cushions;
- spend a little more time with the brace, or the bent elbow, forearm on the belly;
- apply cold to the painful area;
- take pain-relieving medications.
It is common to have pain for a few days or even weeks after the humeral head fracture. The pain can be relieved by various means. This is not a sign of severity, even if it is inconvenient.
See also: Better Sleeping Position with Humerus Fracture?
What complications can occur after a humerus head fracture?
One of the most common complications (though still more the exception than the rule) after a fracture is delayed bone healing, called pseudarthrosis.
But pseudarthrosis is even rarer in humerus head fractures, even if these fractures are complex or displaced. The rate is estimated to be 1.1% for these fractures (Jaeger 2012).
And even in case of delayed or non-union fracture, most people can still regain the use of their arm in daily life.
Even more rarely, in case of surgery, there can be an infection.
Or necrosis of the humerus head (tissues damage).
These are truly extremely rare situations, occurring in people with severe fractures and other risk factors related to their health.
Source: Chandrappa 2017
Some people fully recover their flexibility at the shoulder level. That is, they can lift their arm all the way up to 180° again.

Others recover “only” 100°, 120°, 150° of forward arm elevation. But this is not problematic for daily activities.
The more optimistic you were, with a positive view of your health before having a fracture, the more likely you are to recover well.
Source: Belayneh 2021
What is the recovery time after a humerus head fracture?
Recovery times and healing times will depend on many parameters such as:
- your overall health;
- your genetic predispositions to your body’s healing and recovery abilities;
- the type of fracture and its management.
Here are indicative times based on my experience with patients who have had a radial head fracture (I did not find specific figures on this type of fracture in academic literature).
| Stage | Healing Time (typical timelines) |
|---|---|
| You have significantly less pain | A few days to a few weeks |
| Bone consolidation is completed or well underway | 6 weeks to 3 months |
| Swelling in the arm, bruises disappear | A few days to a few weeks |
| No more need for immobilization, splint | 2 weeks to 2 months |
| Gradual use of the arm for eating, dressing | Several weeks to several months |
| You can drive | 1 to 4 months |
| You can start carrying weight (bags, dumbbells) with the fractured arm | 2 to 5 months |
| You can resume all previous physical and sports activities | 3 to 8 months |
***
Here’s what I wanted to tell you about this! I wish you a very good recovery! Do you have any comments or questions? Your comments are welcome 🙂 !
If you feel the need to learn more about the recovery period after this type of fracture, I wrote this guide in eBook format:
You may also like: Best Sleeping Position for Humerus Fracture
📚 SOURCES
Jaeger M, Izadpanah K, Maier D, Reising K, Strohm PC, Südkamp NP. Frakturen des Humeruskopfes [Fractures of the humerus head]. Chirurg. 2012 Mar;83(3):285-94; quiz 295-6. German. doi: 10.1007/s00104-011-2262-x. PMID: 22406681.
Rodriguez-Corlay RE, Velutini-Becker R, Aguilar-Alcalá LD. Conservative Treatment for Bilateral Displaced Proximal Humerus Head Fracture. Cureus. 2016 Jun 27;8(6):e657. doi: 10.7759/cureus.657. PMID: 27489750; PMCID: PMC4963233.
Launonen AP, Lepola V, Saranko A, Flinkkilä T, Laitinen M, Mattila VM. Epidemiology of proximal humerus fractures. Arch Osteoporos. 2015;10:209. doi: 10.1007/s11657-015-0209-4. Epub 2015 Feb 13. PMID: 25675881.
El-Sayed MM. Surgical management of complex humerus head fractures. Orthop Rev (Pavia). 2010 Sep 23;2(2):e14. doi: 10.4081/or.2010.e14. PMID: 21808705; PMCID: PMC3143970.
Handoll HHG, Elliott J, Thillemann TM, Aluko P, Brorson S. Interventions for treating proximal humeral fractures in adults. Cochrane Database of Systematic Reviews 2022, Issue 6. Art. No.: CD000434. DOI: 10.1002/14651858.CD000434.pub5.
Chandrappa MH, Hajibandeh S, Hajibandeh S. Postoperative outcomes of initial varus versus initial valgus proximal humerus fracture: A systematic review and meta-analysis. J Clin Orthop Trauma. 2017 Jan-Mar;8(1):14-20. doi: 10.1016/j.jcot.2016.09.011. Epub 2016 Sep 29. PMID: 28360490; PMCID: PMC5359510.
Belayneh R, Lott A, Haglin J, Zuckerman J, Egol K. The role of patients’ overall expectations of health on outcomes following proximal humerus fracture repair. Orthop Traumatol Surg Res. 2021 Dec;107(8):103043. doi: 10.1016/j.otsr.2021.103043. Epub 2021 Aug 11. PMID: 34389496.

Written by Nelly Darbois
I enjoy writing articles that answer your questions, drawing on my experience as a physiotherapist and scientific writer, as well as extensive research in international scientific literature.
I live in the French Alps☀️🏔️, where I enjoy the simple pleasures of life (+ I’m a Wikipedia consultant and the founder of Wikiconsult).




