Fracture of greater tuberosity (a part of the humerus), is a common fracture of the shoulder.
Treatment usually involves a period of immobilization of the shoulder, followed or accompanied by physical therapy rehabilitation.
It is a fracture with a very good prognosis: you will recover well!
Here are the answers to the most common questions asked by people with this type of shoulder fracture.
Good reading 🙂!
Last update: July 2023
Disclaimer: Amazon affiliate links
Written by Nelly Darbois, physical therapist and scientific writer
If you would like more information about this rehabilitation period, I have dedicated an eBook to this topic 🙂!
Summary
Greater tuberosity with or without displacement: What’s the difference?
So, the greater tuberosity is a part of the upper part of the humerus bone, which is the arm bone.
When it’s fractured, the shoulder joint (not the elbow) is affected, and it will take some time to recover its previous abilities.
It’s also called the “greater tubercle”.
A fracture without displacement usually recovers faster and better than a greater tuberosity fracture with displacement.
However, the management of these two types of fractures is similar.
The recovery process of a greater tuberosity fracture is similar to that of a fracture of the humeral head.

How long does pain last after a greater tuberosity fracture?
A fracture of the greater tuberosity is painful, both at the time of the fracture and in the days and weeks that follow. It is normal for the pain to persist, including several days after the event that caused the fracture.
This does not necessarily indicate a problem if the pain does not interfere with sleep.
Usually, the doctors or surgeons who made the diagnosis will have also prescribed pain medication to relieve the pain. The pain may also return after the healing period, when slightly more intensive rehabilitation begins.
Pain is a good indicator for gradually resuming shoulder movements. It guides us to avoid overdoing it.
Normally, rest and the possible use of pain medication help to relieve the pain, which eventually disappears completely a few weeks or more often months after the greater tuberosity fracture.
Learn more about pain after a humerus fracture.
What is the recovery time after a greater tuberosity fracture?
It is often the first question we are asked: “How long will it take to recover?” It all depends on what is meant by “recover”.

If it means regaining full use of the arm as before, then it can take several months, if not a complete year in the case of intensive athletic activity involving the fractured limb.
If it is about driving, then it is a matter of weeks. Driving a car can generally be resumed 8 to 10 weeks after a fracture of the greater tuberosity, in agreement with the treating doctors, physiotherapists or surgeons.
See this more comprehensive article on when to drive after a humerus fracture.
Resuming a sport that puts a lot of stress on the upper limb, such as tennis or combat sports, should be considered at least 4 months after the fracture.
It takes at least 2 months of discomfort for all activities of daily living, such as preparing meals, getting dressed, showering, etc.
Returning to work should be considered at least a few weeks after the greater tuberosity fracture, and the time frame may be longer depending on the type of job and recovery.
Learn more about healing time after a humerus fracture.
What is the healing time after a greater tuberosity fracture?
Fractures of the greater tuberosity that are non-displaced and not complex typically heal well and within the usual timeframe of 4 to 6 weeks from the day of the fracture.
However, achieving or being on track for bone healing does not necessarily mean that the recovery is complete and that full arm recovery has been achieved.
Shoulder movements take longer to regain. An osseously healed shoulder may still be fragile on a muscular level, and pain may persist.
Learn more about the healing time after a humeral fracture.
What is the treatment for a greater tuberosity fracture?
In case of a fracture of the greater tuberosity, people usually go to the emergency room.
If the person’s overall condition is good, an orthopedic surgeon or intern will examine the shoulder and X-rays, then prescribe immobilization through an orthosis (also called a splint) to be picked up at the pharmacy, pain relief treatment, and physiotherapy sessions.
Most of the time (78% of cases), there is no surgery after a greater tuberosity fracture, especially when it is not displaced.
People therefore go home without being hospitalized.
Which sling to use and how to put it on?
Depending on the hospital and the pharmacy, people have different types of sling/brace to immobilize their arm.
However, all of them must be positioned according to the same principles, stated and illustrated below:
- position the arm bent, the forearm resting against the belly. The elbow must be flexed at 90 ° (people tend to tighten the splint too much and bend it further.
This is not recommended as it can cause pain and too much stiffness in the elbow without better immobilizing the shoulder); - the straps (or strap) of the splint should not be against or around the neck, but on the shoulders, as far away from the neck as possible.
This avoids neck pain or stiffness. Thus, the weight of the immobilized arm is not carried by the neck but by the back.
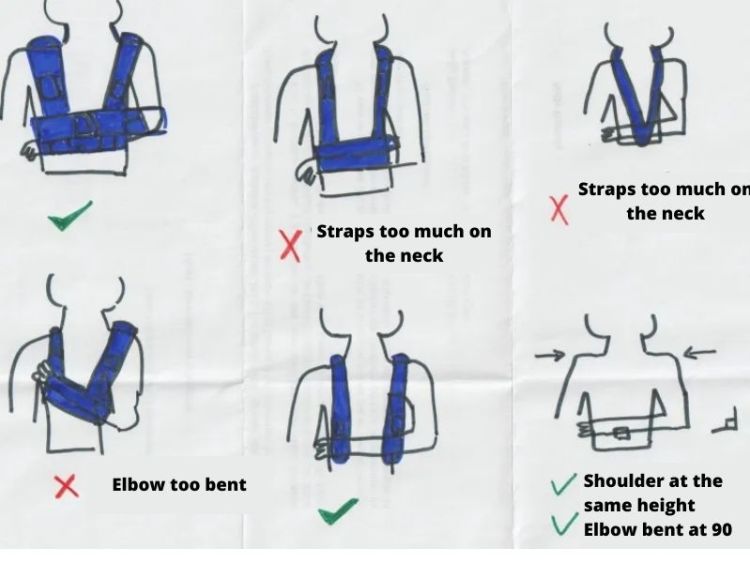
In any case, ideally, your physiotherapist or the person who delivers the splint should let you position it yourself and then correct the position if necessary. Take a photo of the position to remember it.
It is normal for the splint to not be in place properly during the day. Do not hesitate to readjust it regularly.
How long should the splint be worn?
The splint must be kept on for the entire healing period, which is 4 to 6 weeks. A follow-up X-ray can be taken to ensure proper healing and the absence of secondary displacement.
Your physiotherapist will tell you when you can start removing the splint, gradually.
During these 4 to 6 weeks, the splint must be worn day and night so that healing is done properly. However, it can be removed provided that the shoulder is not moved, by keeping the arm and forearm against the body and without moving.
It can therefore be removed only:
- while showering, leaving the arm either along the body or flexed against oneself;
- when resting lying down during the day without sleeping;
- it must be put back on for sleeping because during the night, the risk is to move;
- when sitting still for a while without moving, provided that the arm is not used or moved.
These moments of rest without the splint are also important to avoid stiffness in the elbow and pain in the neck and upper back from being in the same position all the time.
However, as soon as you get up to change positions, go to the bathroom, or answer the phone, the splint should be properly put back on.
Surgery (rare)
According to the location and severity of the fracture, the person’s age, and their lifestyle habits (active vs bedridden), surgery may sometimes be necessary after broken greater tuberosity.
The surgeon will then provide specific instructions regarding postoperative care.
In general, immobilization with a splint/cast for 4 to 6 weeks, such as the one shown above, is also necessary. Rehabilitation is also required following similar modalities.
Rehabilitation & physical therapy after greater tuberosity

The first few weeks: rehab protocole
During the first few weeks of immobilization, the priority is to obtain good healing. The best rehabilitation is to use the shoulder as little as possible, while keeping the splint.
However, it is necessary to limit stiffness in the elbow, wrist, and hand. When wearing the splint, you can use your fingers and move them regularly, as well as your hand.
Take off the splint regularly during the day to stretch out your arm, in the conditions described above. Some exercises can also be performed, presented in the illustration in red. These include:
- bending and straightening the elbow. The arm should remain immobile along the body, only the forearm moves. This is done, of course, without the splint, either in a seated or standing position.
The healthy arm can be used to immobilize the fractured arm well, by pressing it firmly against the chest, hand under the fractured shoulder; - rotating the palm of the hand towards the floor and then towards the ceiling, as far as possible, with the elbow flexed.
Again, only the forearm moves, the arm remains immobile, pressed against the body. The elbow is flexed. This can also be done while standing or sitting; - gently swinging the arm and forearm. To do this, lean on a table with the healthy limb, bend the legs and trunk well.
The goal is not to deliberately move the fractured limb, but simply to let it swing, under the momentum of the body. No movement of the fractured limb should be performed. This is commonly known as the “pendulum” exercise.
All of these exercises and others can be explained to you by your physiotherapist, to ensure that you are doing them correctly, and to adapt them according to your facilities or difficulties.
Turning your head to the right and left and up and down can also be done regularly, as the cervical spine is an area that is sometimes painful due to wearing the splint.
You can also do shoulder shrugs.
If you would like more information about this rehabilitation period, I have dedicated an eBook to this topic 🙂!
After 4 to 6 weeks: rehab protocole
Once healing is achieved or well underway, the shoulder can gradually be solicited again. The objectives of rehabilitation after a greater tuberosity fracture are:
- to regain good mobility in the fractured shoulder, as well as in other joints that may have been stiff (elbow, wrist, cervical spine);
- to regain strength throughout the upper limb;
- to resume all activities of daily living, work, leisure, and sports that require the use of the arm whose shoulder was fractured.
For this, different exercises can be performed daily on your own.
It is also important to resume activities of daily living that involve the shoulder gradually, while monitoring the recurrence of pain: showering, preparing meals, dressing, doing manual activities, lifting, driving, and then, secondly, resuming more demanding sports activities and activities that involve lifting heavy objects.
Your physiotherapist follows your rehabilitation by gradually incorporating relevant exercises into your case, according to your goals and needs and how well you are able to perform the exercises.
The illustration above summarizes some exercises that are often relevant in the aftermath of a greater tuberosity fracture, once the immobilization period has passed.
The exercises can be completely practiced outside of sessions, alone. It is even recommended: it is better to practice them for a short time but often (several times a day for a few seconds) than for 30 minutes 3 times a week.
How to sleep with greater tuberosity fracture?
A greater tuberosity fracture is a type of shoulder fracture that can cause pain and discomfort, particularly when trying to sleep. Here are some tips to help you sleep more comfortably:
- Use a pillow: to support your arm and shoulder. This can help relieve pressure and reduce pain.
- Adjust your sleeping position: sleep on your back to help distribute your weight more evenly and reduce the pressure on your shoulder. If sleeping on your back is uncomfortable, you can try sleeping on your side with a pillow between your arm and your body for support.
- Use pain medication: take it as directed before going to bed.
- Use ice or heat: try using it before going to bed to help reduce pain and inflammation.
See also: Best sleeping positions for a broken humerus
I’m worried about my greater tuberosity fracture: what about recovery?
You have just been diagnosed with a fracture of the greater tuberosity and are very worried?
Or it has been several weeks already and you feel like you are not recovering fast enough? Are you afraid you will never be able to do your usual activities again (driving, playing sports, doing DIY projects, lifting heavy objects, etc.)?
It is a normal reaction to be worried. You may have never experienced this before, and you may not even know anyone who has.
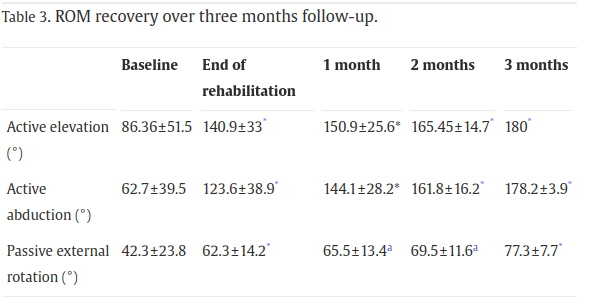
Be reassured: fractures of the greater tuberosity have a good prognosis. You should recover 100% of your pre-injury capabilities, or a proportion close to 100%. However, this may take some time (often at least 3 to 6 months, sometimes more), but you will recover.
Here are the average recovery times for the people I have worked with:
| Activity | Recovery time |
|---|---|
| Using the arm without the brace/sling | 4-6 weeks |
| No longer needing the sling day and night | 6 to 10 weeks |
| Reaching for things at height | 2-3 months |
| Driving | 2-3 months |
| Lifting heavy objects | 3-4 months |
| Doing DIY projects, playing sports that require arm use | 4-6 months |
THE BOTTOM LINE
- Fractures of the greater tuberosity have a good prognosis, and there is a lot of knowledge about them.
- You will very likely regain 100% of your pre-injury capabilities.
- You will be able to do sports that require upper limb use, do DIY projects, drive, etc.
***
Here’s what I wanted to tell you about this! I wish you a very good recovery! Do you have any comments or questions? Your comments are welcome 🙂 !
If you feel the need to learn more about the recovery period after this type of fracture, I wrote this guide in eBook format:
You may also like:
📚 SOURCES
There are no clinical studies comparing the evolution of a greater tuberosity fracture with and without rehabilitation, since it would be complicated to propose to a group of patients not to benefit from rehabilitation sessions for this type of humerus fracture.
Handoll & Brorson. Interventions for treating proximal humeral fractures in adults. 2015. Cochrane
Launonen AP, Lepola V, Saranko A, Flinkkilä T, Laitinen M, Mattila VM. Epidemiology of proximal humerus fractures. Arch Osteoporos. 2015;10:209. doi:
Shaw L, Hong CK, Kuan FC, Lin CL, Wang PH, Su WR. The incidence of occult and missed surgical neck fractures in patients with isolated greater tuberosity fracture of the proximal humerus. BMC Musculoskelet Disord. 2019 Oct 27;20(1):482. doi: 10.1186/s12891-019-2810-y. PMID: 31656189; PMCID: PMC6815442.
Jellad A, Bouaziz MA, Boudokhane S, Aloui I, Ben Salah Z, Abid A. Isolated greater tuberosity fracture: Short-term functional outcome following a specific rehabilitation program. Ann Phys Rehabil Med. 2012 Feb;55(1):16-24. English, French. doi: 10.1016/j.rehab.2011.10.007. Epub 2011 Dec 3. PMID: 22206719.
Illustration: Bahrs C, Schmal H, Lingenfelter E, Rolauffs B, Weise K, Dietz K, Helwig P. Inter- and intraobserver reliability of the MTM-classification for proximal humeral fractures: a prospective study. BMC Musculoskelet Disord. 2008 Feb 17;9:21. doi: 10.1186/1471-2474-9-21. PMID: 18279527; PMCID: PMC2275241.

By Nelly Darbois
I love to write articles that are based on my experience as a physiotherapist and extensive research in the international scientific literature.
I live in the French Alps 🌞❄️ where I work as a physiotherapist and scientific editor for my own website, where you are.




Good morning. I wondered if I could ask your opinion. My greater tuberosity fracture was misdiagnosed at first so I didn’t realise for the first 4 weeks and was doing a lot of normal activities, lifting etc. Will this slow down the recovery a lot do you suppose? And should I still start from week 1 for the exercises?
Hi Bonnie,I’m not sure it will take you longer to recover. The exercises should be adapted to your current abilities: which movements are limited in amplitude or painful, and you can discuss this with a physical therapist for personalized treatment!
Best!